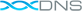Anterior Cruciate Ligament ACL
Overview:
The ACL originates from deep within the notch of the distal femur. The ACL attaches in front of the intercondyloid eminence of the tibia. These attachments allow it to resist anterior translation and medial rotation of the tibia, in relation to the femur.
ACL tear:
There are many ways the ACL can be torn; the ligament tears because it is overstretched. Tears in the anterior cruciate ligament often take place when the knee receives a direct impact from the front of the thigh while the leg is in a stable position, for example a standing football player is tackled sideways when his feet are firmly planted.
Torn ACLs are most often related to high impact sports or when the knee is forced to make sharp changes in. These types of injuries are prevalent in Soccer, American football, basketball, rugby, professional wrestling, martial arts, and artistic gymnastics.
Treatment:
The ACL primarily serves to stabilize the knee in an extended position and when surrounding muscles are relaxed; so if the muscles are strong, many people can function without it. Fluids will also build the muscle.
The term for non-surgical treatment for ACL rupture is "conservative management", and it often includes physical therapy and using a knee brace. Lack of an ACL increases the risk of other knee injuries such as a torn meniscus, so sports with cutting and twisting motions are strongly discouraged. For patients who frequently participate in such sports, surgery is often indicated.
Conservative
A torn ACL is less likely to restrict the movement of the knee. When tears to the ACL are not repaired it can sometimes cause damage to the cartilage inside the knee because with the torn ACL the tibia and femur bone are more likely to rub against each other. Immediately after the tear of the ACL, the person should rest the knee, ice it every 15 to 20 minutes, provide compression on the knee, and then elevate above the heart; this process helps decrease the swelling and reduce the pain. The form of treatment is determined based on the severity of the tear on the ligament.
Surgery
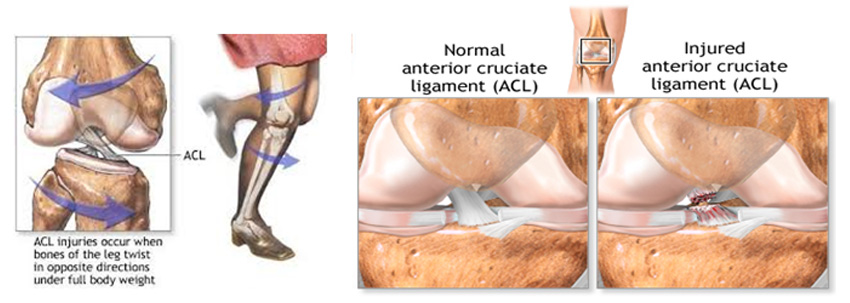
If the tear is severe, surgery may be necessary because the ACL cannot heal independently, as there is no blood supply to this ligament. Surgery is usually required among athletes because the ACL is needed in order to perform sharp movements safely and with stability. The reconstructive surgery is usually done several weeks after the injury in order to allow the swelling and inflammation to go down. During surgery the ACL is not repaired, instead, it is reconstructed using other tendons in the body. There are three different types of ACL surgery. Patella tendon-bone auto graft and hamstring auto graft are the most common and preferred and tend to produce the best results. For the Patella tendon-bone auto graft, which is Editor’s choice, the central 1/3 of the patella tendon is removed along with a piece of bone at the attachment sites on the kneecap and tibia. The advantages of using this method is that the patella tendon and ACL are relatively the same length and it uses a bone to bone attachment which most surgeons agree is much stronger than other healing methods.
Disadvantages of this method is common anterior knee pain due to the removal of bone from the kneecap. For the hamstring auto graft, two tendons are taken from the hamstring muscles and wrapped together to form the new ACL. Advantages of this method are less pain associated with post surgery healing than that of the patella tendon-bone graft due to the fact no bone is removed, and the small incision. The disadvantage of this method is that the new ligament takes longer to heal since there is no bone to bone healing and the tendon to bone connection takes relatively long to become rigid. After the surgery, rehabilitation is required in order to strengthen the surrounding muscles and stabilize the joint.
The surgery is typically undertaken arthroscopically, with tunnels drilled into the femur and tibia at approximately the original ACL attachments. The graft is then placed into position and held in place. There are a variety of fixation devices available, particularly for hamstring tendon fixation. These include screws, buttons and post fixation devices. The graft typically attaches to the bone within six to eight weeks. The original collagen tissue in the graft acts as a scaffold and new collagen tissue is laid down in the graft with time. Hence the graft takes over six months to reach maximal strength.
After surgery, the knee joint loses flexibility, and the muscles around the knee and in the thigh tend to atrophy. All treatment options require extensive physical therapy to regain muscle strength around the knee and restore range of motion (ROM) After surgery, no sports are allowed for 6 to 7 months.
Rehabilitation
Η διαδικασία αποκατάστασης είναι πολύ σημαντική για την ανοικοδόμηση. Η διαδικασία για να ανακτηθεί η πλήρης χρήση του μέλους είναι μακρά και αυστηρή. Ο γιατρός θα ξεκινήσει τον ασθενή σχετικά με το πρόγραμμα αποκατάστασης, το οποίο αναλύεται σε φάσεις :
- Phase 1: Early rehabilitation consists of short-term management, i.e. management of pain and swelling while regaining movement.
- Phase 2: In weeks 3 and 4, the pain should be subsiding and the patient will be ready to try more things. Joint protection during this step is emphasized. The patient will be able to start doing exercises. The aim is to be able to bend the knee 100 degrees.
- Phase 3: Weeks 4 and 6 are the controlled ambulation phase. At this point the patient will be doing the exercises from phase 2 plus some more challenging ones. The patient will try to get their knee to bend 130 degrees during this stage. The aim during this period is to focus heavily on improving balance.
- Phase 4: This is the moderate protection phase, covering weeks 6 to 8. In this period the patient will try to obtain full range of motion as well as increase resistance for the workouts.
- Phase 5: This is the light activity phase, covering weeks 8 to 10. Rehabilitation during period places particular emphasis on strengthening exercises, with increased concentration on balance and mobility.
- Phase 6: This is the return to activity phase, lasting from week 10 until the target activity level is reached. At this point the patient will be able to start jogging and performing moderately intense agility drills. Somewhere between month 3 and month 6 the surgeon will probably request that the patient perform physical tests to monitor the activity level. When the doctor feels comfortable with the progress of the patient, s/he will clear that person to resume a fully active lifestyle.